My name is Charity Damron, and on October 8th, 2019, I underwent a life-changing medical procedure called a vertical sleeve gastrectomy, or VSG for short. The eighteen months that followed have been a whirlwind—a mixture of complications, hospital stays, victories (both on and off the scale), more surgeries, intense joys, deep pains, and so much more. It’s hard to even put into words how my life has transformed, but I will do my best. To truly understand how we got here, we need to start at the very beginning—back in 1988.
I was born two months premature, weighing 8 pounds, 13 ounces. From virtually the start of my life, I was considered morbidly obese. While I don’t put much stock in the Body Mass Index (BMI) as a measure of health, it’s medically used to indicate risk—and mine consistently fell in the obese to morbidly obese range. Throughout childhood and adolescence, I was always severely overweight, yet very active. I played sports, participated in marching band, and kept busy in school activities. Despite all of this, the scale never seemed to reflect my efforts.
Being obese didn’t mean I was unhealthy. In fact, I was generally very healthy “for being obese,” as doctors used to say. I had no major weight-related medical issues, and my weight never seemed to stop me from living a full life—or so I thought. It wasn’t until my husband, Cody, and I decided to start a family that I realized just how much my weight might be holding me back.
We began trying for a baby in 2014, but I had a long history of irregular menstrual cycles. Back in 2011, I underwent a dilation and curettage (D&C) procedure due to persistent bleeding caused by uterine polyps. I didn’t have a proper cycle for almost a year afterward, and since then, my cycles were inconsistent at best. After three months of unsuccessful attempts to conceive and multiple tests from my OBGYN, I was officially diagnosed with polycystic ovarian syndrome (PCOS) in 2014.

We attempted three rounds of fertility treatments, which wreaked havoc on my hormones and triggered intense mood swings each cycle. Eventually, Cody and I had a serious conversation about the reality that PCOS might prevent us from ever conceiving naturally, and that my weight could be a contributing factor.
I decided to try losing weight again on my own. Over the years, I had successfully lost 50–75 pounds multiple times, only to eventually hit a wall and regain the weight despite consistent effort. Hormonal issues made the process more difficult, but I was determined. Over the next few years, I once again shed 50 pounds. By December 2018, we decided to resume fertility treatments, with Cody also being checked to ensure everything was fine on his end—which it was.
Unfortunately, the treatments were unsuccessful once again. I began gaining weight back, even while staying disciplined with diet and exercise. By March 2019, feeling frustrated and at my wit’s end, I attended a seminar at my local hospital about weight-loss surgery. I had been skeptical—some people I knew had regained their weight after surgery, while others had been successful and happier. I didn’t know where I would land, and I wasn’t sure I wanted surgery to fix something doctors had always told me I could do on my own.

During the seminar, a single slide changed my entire perspective. It listed medical comorbidities associated with obesity and explained how weight-loss surgery could improve or even resolve them. PCOS—and its impact on fertility—was among them. For me, this wasn’t about wanting to be thin. I was happy being fat. My husband loved me, my friends and family loved me, and I had been healthy for most of my life. But the possibility that surgery could improve my fertility, and perhaps give us the chance to have our own biological child, sold me.
Insurance required six months of medically supervised diet and exercise before surgery. I began this journey in March 2019 at 301 pounds (after previously hitting a personal high of 327 pounds in October 2018). Over the next six months, I fluctuated about 20 pounds, and by the start of my three-week pre-op diet in September, I weighed 300 pounds. By surgery day, October 8th, 2019, I weighed 271 pounds.

Those six months were transformative in more ways than one. Cody and I became licensed foster parents and welcomed twin 13-month-olds into our home in May 2019. By July, we added Chiara, an Italian foreign exchange student, for the school year. Our “do-whatever-we-want” lifestyle disappeared overnight, replaced with constant activity and responsibility. Parenting toddlers, especially two at once, was overwhelming—but somehow, we survived and thrived.
As a parent, I quickly realized that keeping up with toddlers was physically exhausting. Running, playing, and chasing them highlighted the limitations my body faced. The surgery now became not only about fertility but about the stamina to keep up with my growing family.
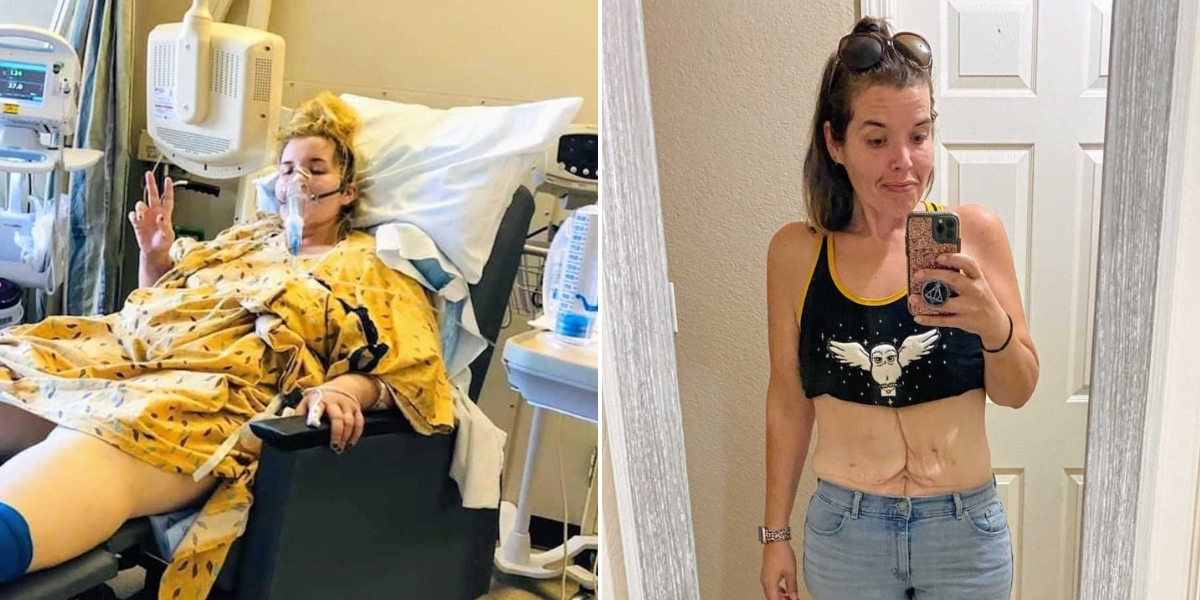
Just days before surgery, on October 4th, we closed on our dream property. Then, on October 8th, I went in for my VSG. About 70–80 percent of my stomach was removed, leaving me with what’s called a “sleeve.” Initially, my surgery and recovery were textbook. I stayed an extra night in the hospital for safety but was walking every 20–30 minutes, hydrating, and feeling optimistic. In six weeks, I returned to work, ran a school-wide music program, and even went on a family trip to San Diego. I had already lost almost 30 pounds since surgery and over 80 pounds overall.
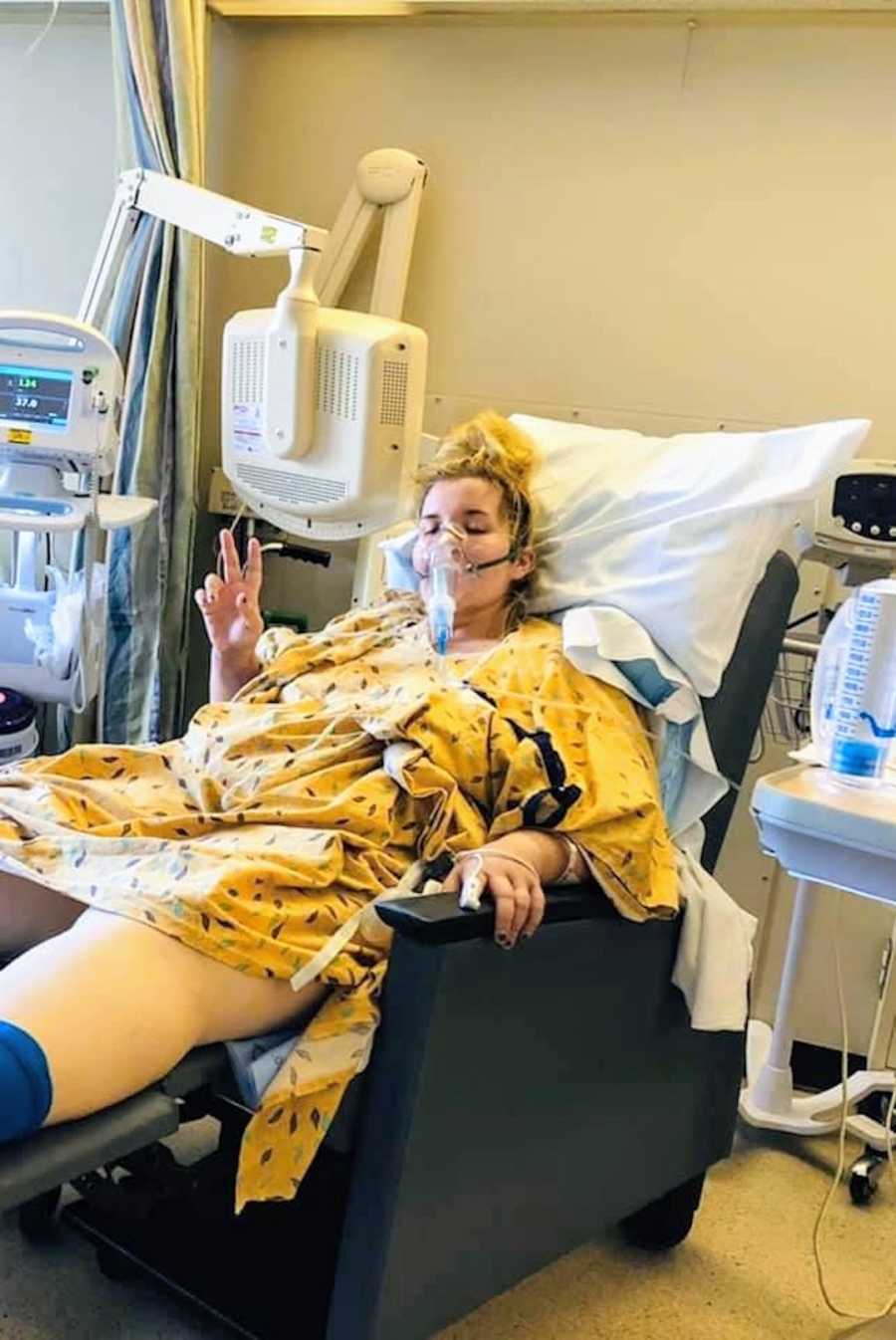
Then, things took a dramatic turn. In late November 2019, I developed chills, fever, nausea, and severe weakness. Initially diagnosed with the flu, I was sent home with IV fluids. But my symptoms escalated—heart racing, uncontrollable shivering, and intense pain in my groin, abdomen, chest, and shoulders. By the early hours of November 24th, I knew something was seriously wrong. My husband rushed home, and we went straight to the ER.
I was in septic shock. My new sleeve had developed a leak at the junction with my esophagus, allowing contents to spill into my abdomen. I could have died within minutes if I had waited any longer. Emergency surgery stabilized me temporarily, but I needed to be transferred by helicopter to a larger hospital equipped for high-risk cases.
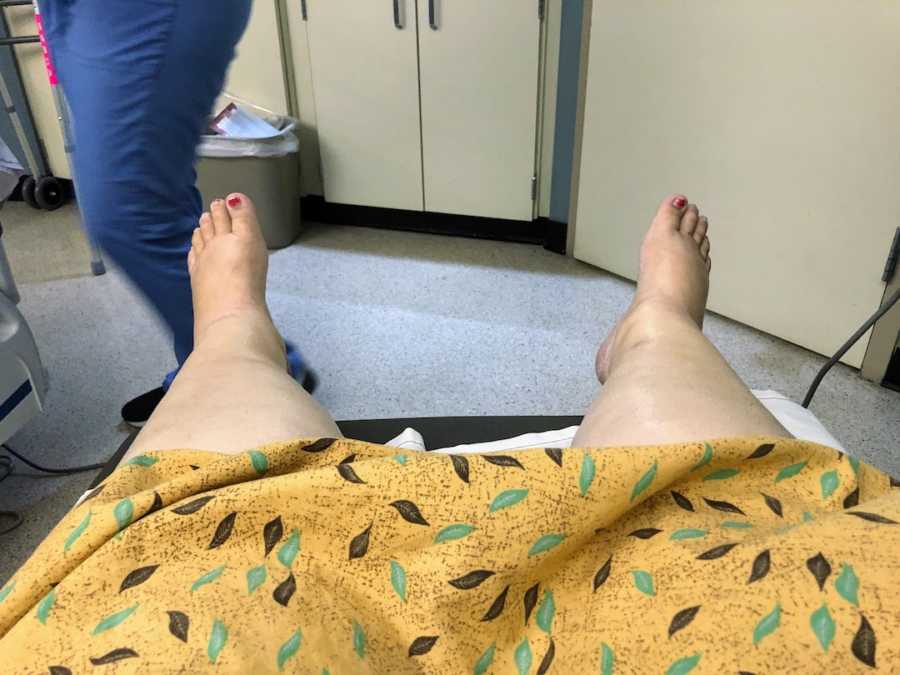
At Banner University Medical Center in Phoenix, I woke in the ICU to swollen legs and a ladder-like line of staples holding my abdomen together. My parents were by my side. The following three weeks were a blur of procedures: multiple CT scans, a thoracentesis for a collapsed lung, swallow studies, two upper GI endoscopies, six abdominal drains, and a PICC line for total nutrition and medications. I remained NPO—no food or water for nearly two months.
The hospital stay was mentally and physically grueling. I suffered panic attacks, had to relearn how to walk, and struggled with anxiety that lingers to this day. My parents stayed the first week, and friends helped care for our children. When I finally returned home on December 14th, I was still connected to my PICC line and drain, navigating a challenging new normal.
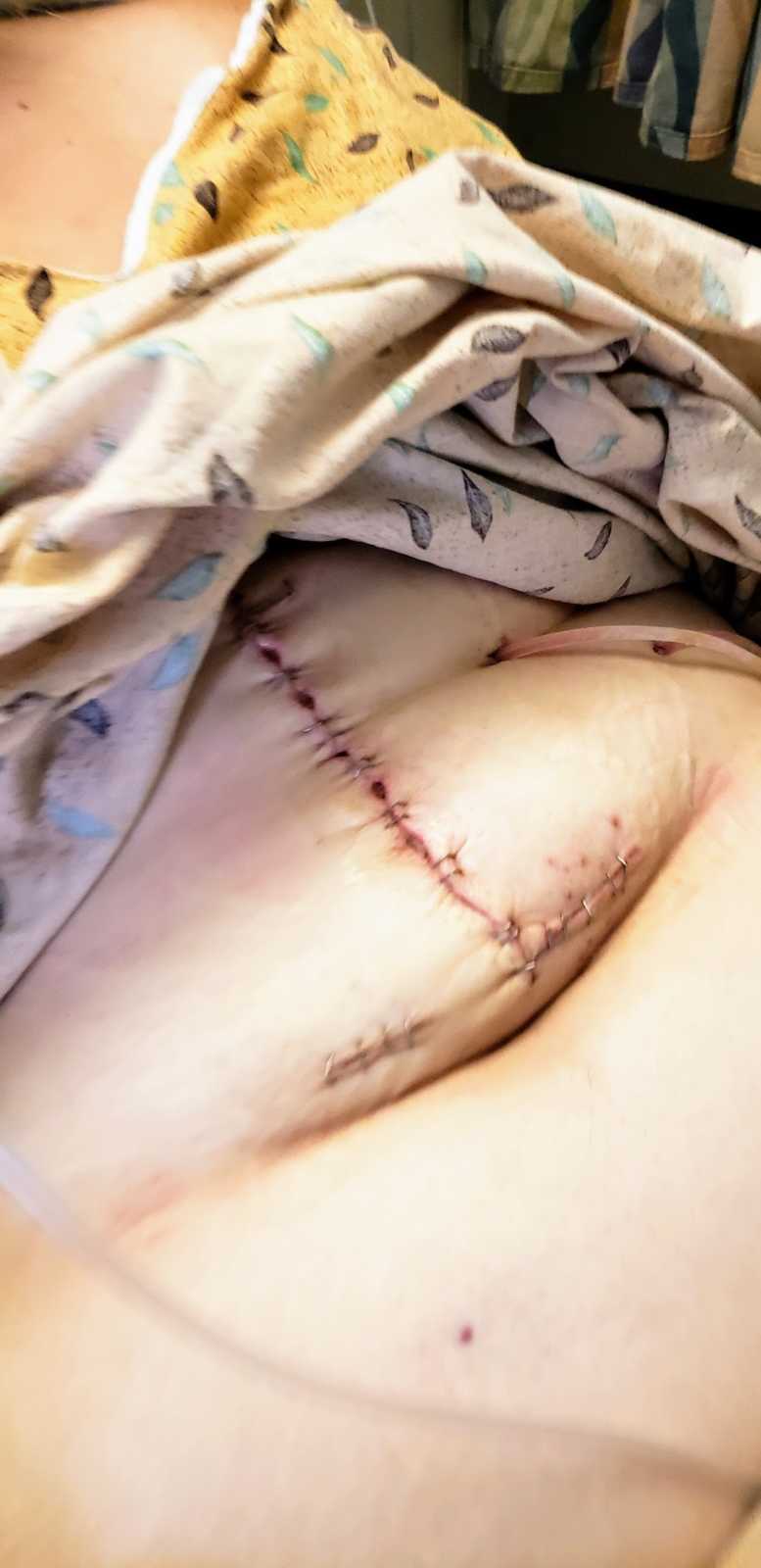
Recovery was slow. I gradually transitioned to clear liquids, then full liquids, and finally soft foods. By February 17, 2020, my PICC line was removed, and I could take all nutrition by mouth again. My energy returned, and I could play with my twins and care for our newborn foster child, all while navigating COVID restrictions.
In July 2020, I experienced back and shoulder pain, later confirmed as another sleeve leak. This time, the leak was detected early, and I stayed a week in the hospital, receiving a new drain and PICC line. My surgeon explained I would eventually need a gastric bypass revision to prevent future leaks. Pre-op, I ate a soft diet for four months while preparing for high-risk surgery. Gallstones were also discovered, necessitating gallbladder removal.

On December 1, 2020, I underwent a laparoscopic gastric bypass revision. My collapsed sleeve was repaired, allowing food to pass correctly and preventing further leaks. Recovery was smooth, and by January 2021, I returned to normal diet and exercise. A brief scare in February 2021—life-flighted for suspected leak—turned out to be an abdominal staph infection, which was far easier to manage.
By April 2021, I was four months post-revision and eighteen months from my original surgery. I fluctuate between 160–165 pounds, down from a high of 327, and wear size 8 jeans and XS/S tops. My BMI went from 53 to about 25. More importantly, I can play with my twins for hours, feel confident in my skin, and have a healthier relationship with food.
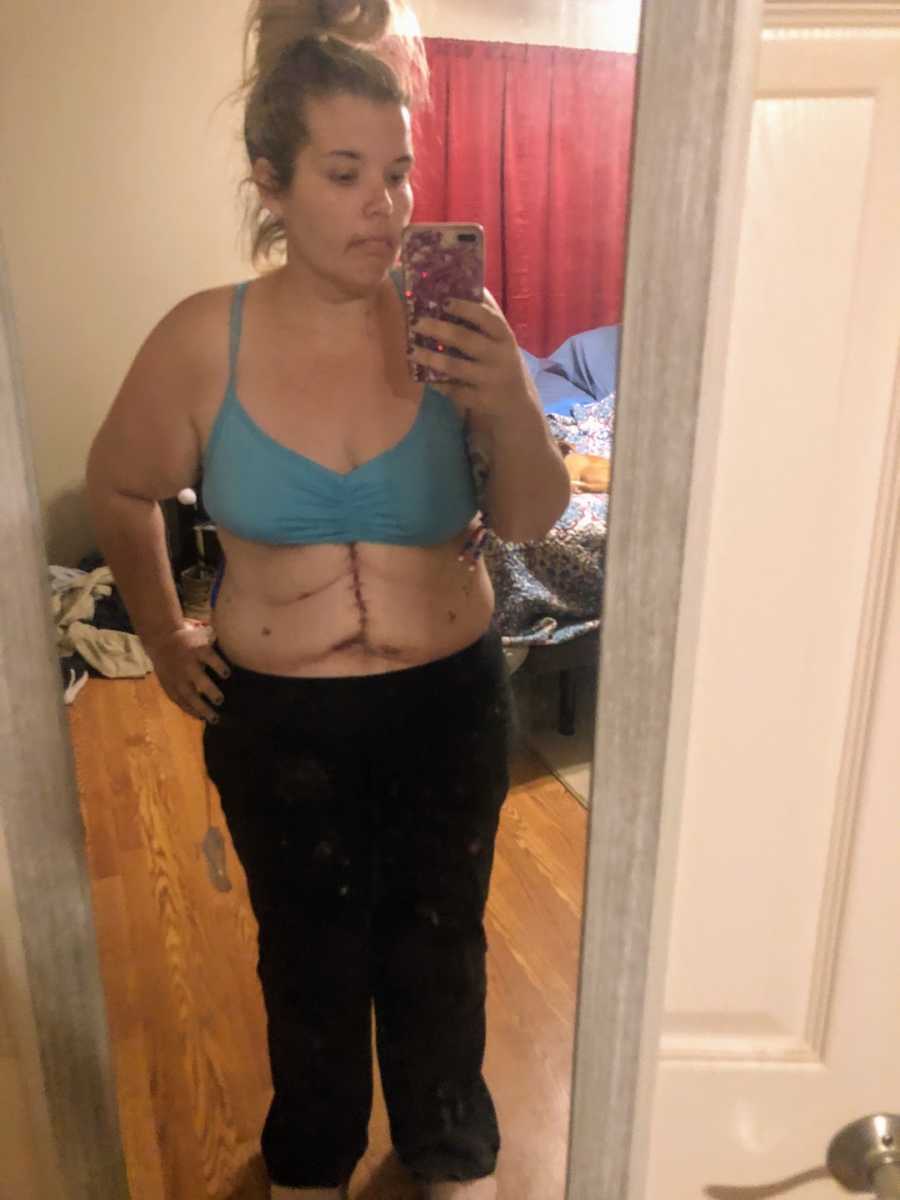
Do I regret any of it? Absolutely not. The journey has been difficult, even traumatic at times, but it has given me a new lease on life. My scars tell my story, a roadmap of resilience, healing, and growth. I continue to share my journey online, hoping to normalize and destigmatize weight-loss surgery and inspire others to pursue health and happiness. Life is unpredictable, challenging, and beautiful—and I finally feel ready to embrace it fully.