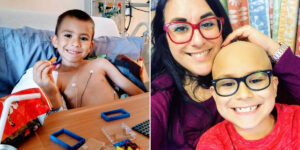
I suffered 22 miscarriages before, yet somehow it felt like I got pregnant every other month. Even in months we avoided it, I still found myself with that familiar two-line result—like the time I got pregnant on day 29 of my cycle. Each loss was no easier than the last, yet we became numb to this cruel, repetitive cycle: get pregnant, hope, lose it. Some pregnancies lasted a little longer than others, but most followed a predictable, almost clockwork rhythm. Over time, we started planning our lives around potential miscarriages—canceling plans, avoiding big events, and making zero commitments, just in case.
So when I felt the all-too-familiar cramps on Friday, March 30, 2018, I knew I had to go to urgent care to check my HCG levels. I had a sinking feeling that I was about to lose another baby. And the timing couldn’t have been worse—Sunday, April 1st, was not only Easter but also my birthday. If I was miscarrying again, I needed to cancel the entire weekend, especially my birthday.
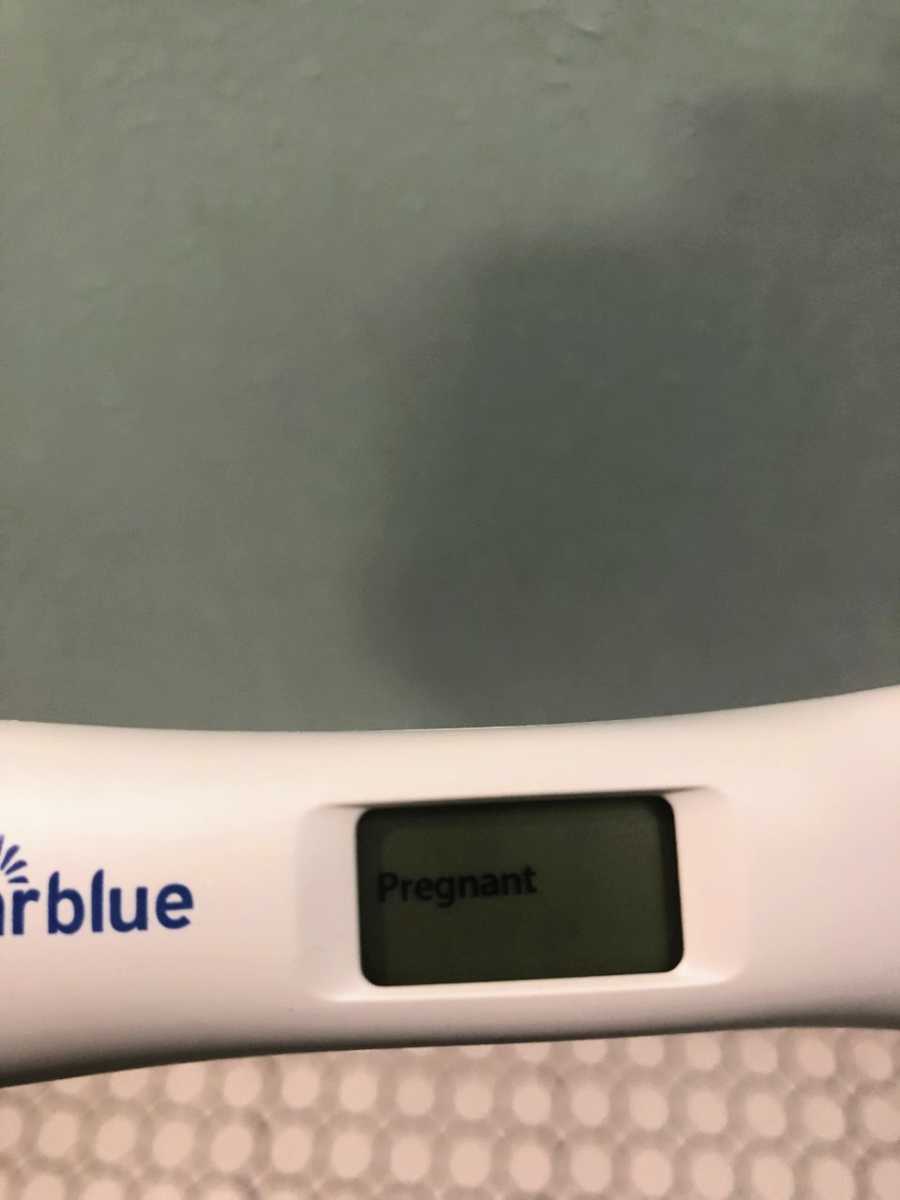
We arrived at urgent care around 3 p.m., and they quickly performed an ultrasound. My heart dropped, then soared with relief—except for one horrifying detail: the baby was growing in my fallopian tube. The urgent care doctor immediately contacted my fertility doctor, who insisted I be rushed to the hospital by ambulance. Hours passed as we waited. I just wanted to drive there myself, but the risk was too great—I could die if I tried to get there without medical supervision.
By midnight, we finally arrived at the hospital. It was chaos—hallways lined with gurneys, patients shuffled around like furniture. I lay alone on a gurney, bumped and shifted repeatedly, feeling both humiliated and strangely comforted. Every minute in that hallway meant my baby was still alive.
After about an hour, I was moved into a room, and my husband joined me. Soon, two student doctors came in, blunt and clinical: “You have an ectopic pregnancy. You have to terminate. You have two options: surgery or a methotrexate injection.” I broke down, tears streaming as they stood silently, clearly uncomfortable with my pain. They expected me to decide immediately. I pulled the blanket over my head and waited, frozen in despair, until they finally left.
Through tears, I told my husband over and over that I wanted to keep this baby. “How can they ask me not only to terminate but also to choose how?” I asked him. “Do they not understand how long we’ve waited for a baby that sticks?” I knew I had no real choice—refuse treatment, and I could die—but understanding that didn’t make it any less devastating.
I wanted surgery to be over with, but after listening to the doctors, my fertility specialist, and my husband, I chose the methotrexate injection. It promised to save my ovary and tube and, most importantly, my life. Around 5 a.m., I received the injection and was sent home with instructions to wait it out.

The next day, I rested, processing the previous fifteen hours of hell. I felt broken beyond measure, but I also knew I would survive. I had lost so many babies before, and somehow, in this cruel routine, I had adapted. My blood was checked every 48 hours to monitor HCG levels, confirming the pregnancy had ended. The numbers dropped steadily, which my doctor described as “impressive.” Those words—clinical and detached—were somehow comforting; I was no longer at risk of dying. Slowly, I returned to normal life, focusing on my kitchen remodel and my 12-year-old son’s homework. I thought the worst was over.
But the real trauma was yet to come.
Exactly two weeks later, I woke up with the worst pain I’d ever felt. Initially, I tried to convince myself it couldn’t be the pregnancy. Crawling to the bathroom, I had a creeping feeling that something was terribly wrong. Once back in bed, I prayed: “God, if this is serious, please let me know.” Almost immediately, I felt my strength leave me. My husband woke to the sight of me pale, drenched in sweat, and barely conscious. Panic-stricken, he carried me to the car and drove to the hospital himself, refusing to wait for an ambulance.

At the hospital, staff initially dismissed me. “Probably an ovarian cyst,” one doctor said without examination. I insisted this wasn’t like the cysts I’d experienced before. We demanded my doctor be contacted. Eventually, I underwent an ultrasound. To my shock and relief, I saw the tiny, unmistakable heartbeat. “That’s our baby,” I whispered. The baby I thought I had lost was still alive.
But the methotrexate had failed. The baby continued to grow, rupturing my tube and putting my life in immediate danger. Emergency surgery was the only option. On April 13, 2018, I lost my baby for a second time, and this loss—the 23rd—broke me completely. The grief was unlike anything I had experienced before. Unlike my previous losses, this trauma consumed me. For over a year, I was trapped in darkness. Each day was a battle just to function—getting out of bed, holding a conversation, even physical touch felt impossible. I forced myself to go through the motions for my son, knowing he depended on me.
On Mother’s Day that year, I tried to hide my emptiness at the beach. My swollen stomach and fresh scars were constant, painful reminders of what should have been. I felt like a failed mother, a failing wife, and for the first time, I had no idea why I was broken. Words like sadness, grief, or heartbreak couldn’t capture the depth of what I felt.

After a year of numbness, I woke one morning and realized I could survive this. I named it—depression—and began to confront the trauma I had buried for so long. Healing began when I understood that baby 23 didn’t break me alone. I had never allowed myself to grieve the 22 losses before. I had forced myself to be strong, to return to “normal,” and to suppress my pain, all while society expected me to move on. That compounded grief had been suffocating me for years.

Through this journey, I’ve grown stronger, more compassionate toward myself, and more intentional about living fully. I’ve learned to honor each of my angel babies, to acknowledge their presence in my life, and to love my family without guilt. I can finally watch my son grow, enjoy the beach, and embrace moments of joy without letting grief overshadow them.
I still experience waves of sadness, anger, and doubt. I always will. But now I allow myself to be present in each wave, to process my emotions, and to remind myself that it’s okay to not be okay. One in four of us has endured losses like mine, a club we never chose. Yet being part of this club also means we are not alone. We deserve to grieve fully, to cry, to heal, and to honor the lives we lost—our heartbreak is real, valid, and worthy of love and attention.