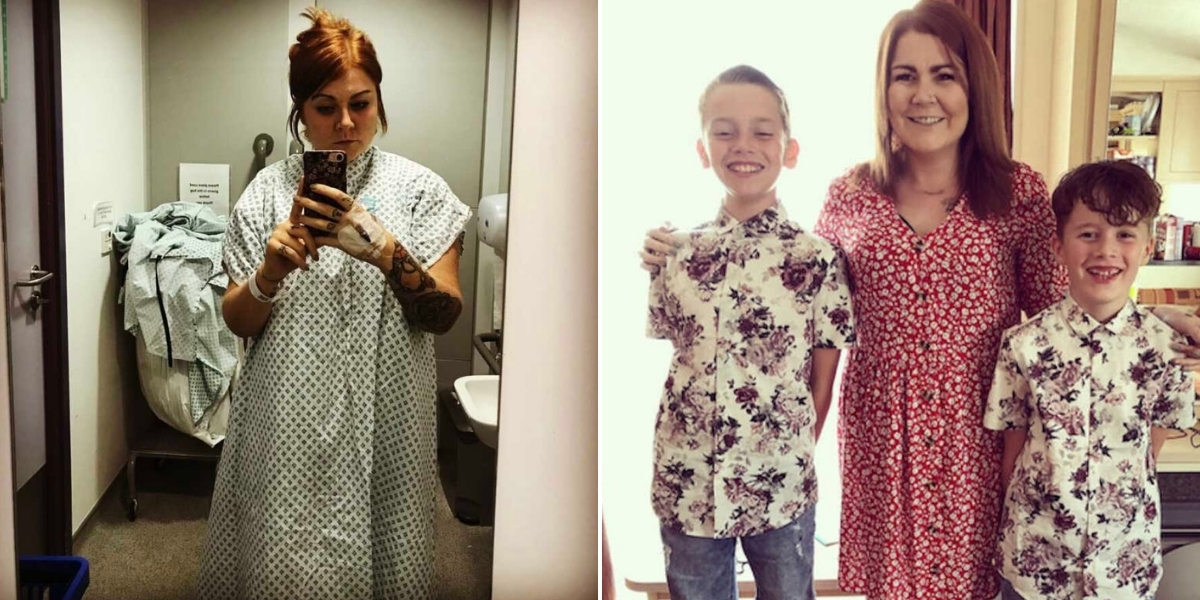
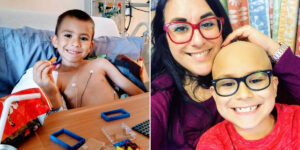
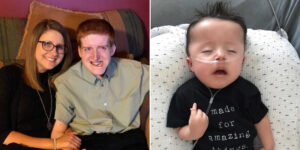
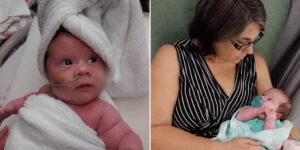
I didn’t always live with Lupus. Like so many others, it surfaced after a deeply traumatic time. During my second full‑term pregnancy, my relationship with my partner fell apart. I was five months along, caring for my 2‑year‑old, working part‑time, and clinging to hope while doctors monitored my baby constantly. Noah was considered a “lazy” baby — his heartbeat dipped often, and he moved far less than doctors liked. For the last 12 weeks, I was at the hospital every other day, exhausted and terrified. In the end, they induced my labor, and despite everything, Noah arrived — tiny, beautiful, and healthy.

When Noah was around 2 months old, my body began to fail me. I felt like I hurt everywhere. The fatigue was crushing, and my motivation disappeared. Doctors brushed it off as post‑natal depression because I’d been through so much, but deep down I knew it wasn’t that. My mom finally came with me and insisted they take it seriously. Blood tests revealed an autoimmune condition, hypothyroidism, and suspected Hashimoto’s thyroiditis. I was prescribed thyroxine and told I’d likely take medication for life but could still live “normally.” What I didn’t realize then was that this was only the beginning — it would take four more years to discover I actually had Lupus.

Even with the correct thyroid dose, I never felt right. My muscles and joints constantly ached, and I needed sleep every chance I got. Simple chores wiped me out. After family outings, I’d need days to recover. Friendships faded because I kept canceling plans — lunches, shopping, nights out — everything took more energy than I had. All of my strength went toward raising my boys and keeping my part‑time job. Then the rashes began: angry, inflamed patches across my face — what I’d later learn was a malar or “butterfly” rash. Doctors assumed eczema and tried creams that either burned or did nothing. I was constantly back in the clinic with painful skin, UTIs, and unexplained body pain.
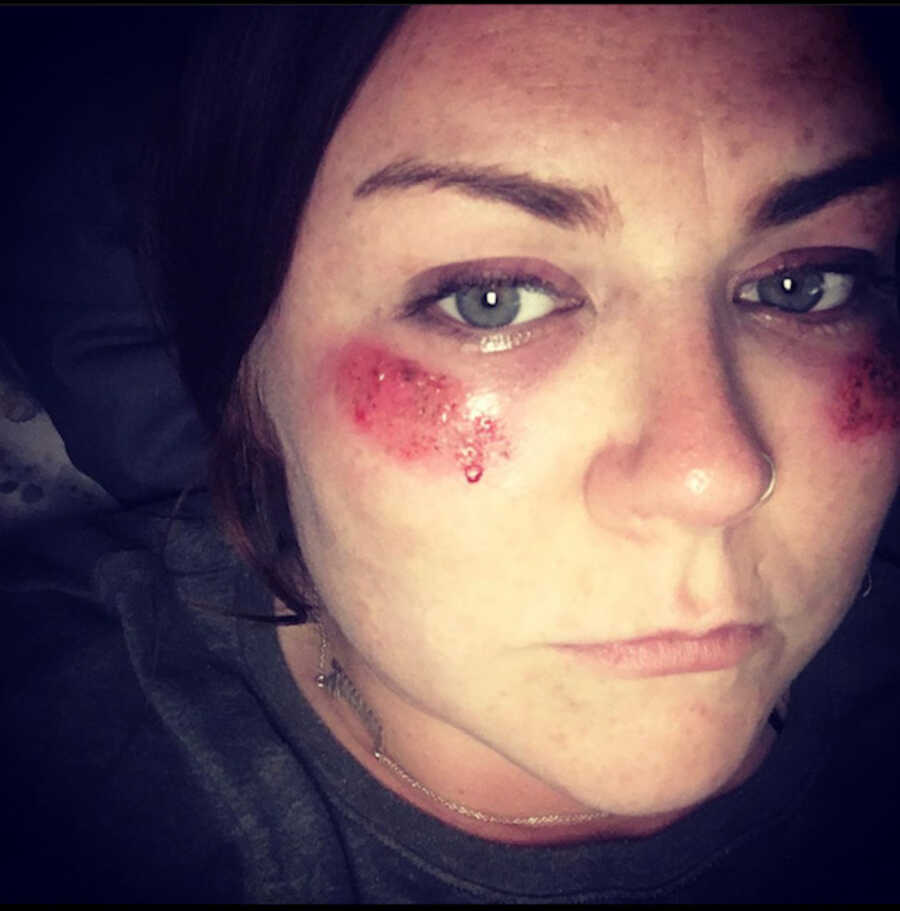
One day, I saw a different doctor — and everything shifted. He actually listened. He didn’t blame depression or my thyroid. He suggested more bloodwork and referred me to a rheumatologist because my symptoms pointed to Lupus. I knew my great aunt had Lupus, but I didn’t really understand what that meant. I made the mistake of Googling it and convinced myself my life was over. The fear alone made me feel worse, and over time I learned stress is one of my biggest flare triggers.
After three months, the rheumatologist confirmed it: I had Lupus, specifically SLE — a chronic illness where the immune system attacks healthy tissues, including skin, joints, and organs like the kidneys and heart. I felt devastated, yet relieved to finally have an answer. Treatment began with immune‑suppressing medications, but finding the right combination was slow and unpredictable. Eventually I learned my Lupus mainly attacks my skin, muscles, joints, heart, kidneys, spine, and brain.
Two years into treatment, things spiraled. I developed severe back pain, and within weeks I lost bladder sensation. I couldn’t urinate despite the agony. At A&E, a scan showed my bladder was full, but after I managed to go a little, they sent me home, assuming a trapped nerve. Two days later, I was worse, limping and losing feeling in my left leg. Another emergency visit, an MRI, and suddenly everything moved fast — I had Cauda Equina syndrome and needed urgent transfer for emergency spinal surgery. I was terrified, especially after being warned paralysis was a risk.
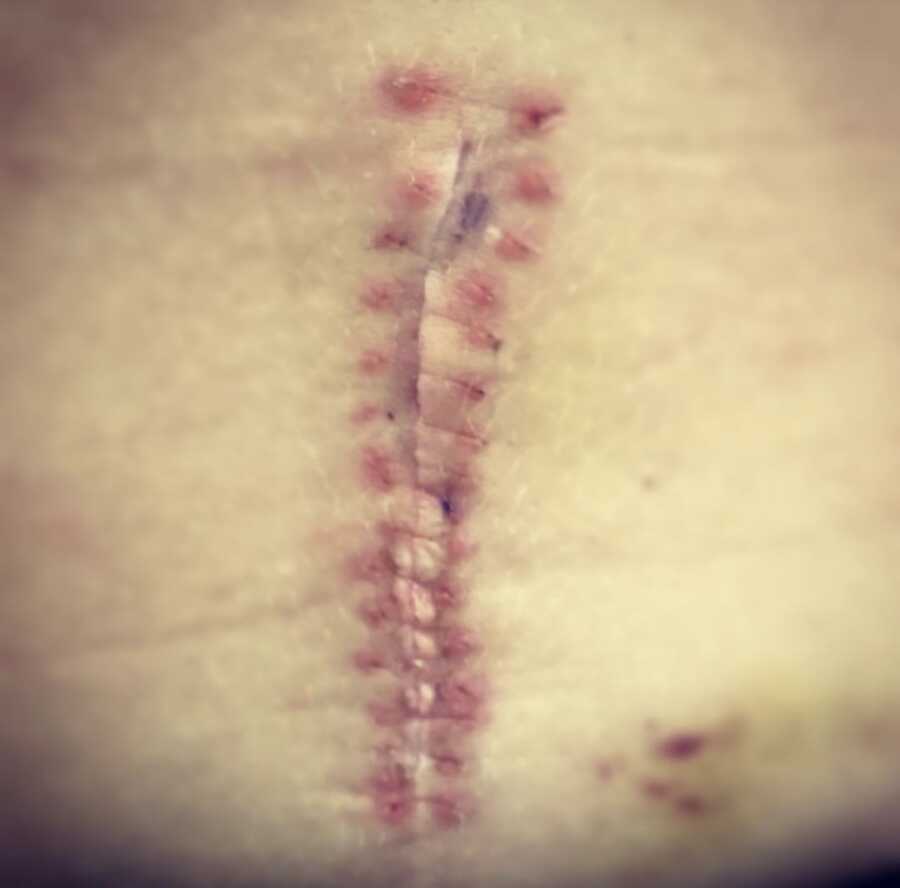
The next day, I woke in the ward with tubes everywhere, unable to sit up. Doctors explained a piece of my spinal cord had been “nicked,” and I needed to stay flat so the fluid didn’t burst the stitches. I also had a slipped disc pressing on my nerves — the reason I lost bladder and leg sensation. If they hadn’t operated, it could have been catastrophic.
When I finally stood, I nearly fainted. My leg dragged, and nurses reassured me nerves might heal with time. I moved in with my parents temporarily, still unable to feel my bladder and learning how to self‑catheterize. Over time, I taught myself to walk again. A year later, scans showed residual disc material, so surgeons tried a second operation — but it didn’t help. My specialists eventually agreed my Lupus had likely attacked my spine. Today, I still limp and rely on crutches, a walker, or a wheelchair for distance — but I’m grateful I can walk at all.
Lupus has taken so much. Alongside it, I live with secondary autoimmune conditions, Osteoarthritis, and Trochanteric Bursitis. I take around 30 pills a day, have constant blood tests, and see my rheumatologist every eight weeks. Mentally, it’s heavy. I’ve cried, felt terrified, and worried I’m a burden — especially on the days my children end up caring for me. I think about the future, the moments I might miss, and sometimes wonder why this became my life.

But I’m also blessed. My family and friends are incredible, and my boys, Jude (13) and Noah (11), amaze me every day. They don’t remember me before illness, which in a strange way brings peace. When I’m unwell, we build nests on the sofa, color, or picnic in the living room. When I’m well, we chase beach days and park adventures. I’m honest with them about appointments and symptoms because I want them to understand, and I see how it’s shaping them into compassionate young men.

Still longing for someone who truly understood, I started my Instagram, @lollyandlupus — and it changed everything. I found a community that “gets it.” I can share openly, ask questions, vent when plans turn into bed days, and lean on friends who live this life too. Our little “lupus lovelies” group chats daily, meets up when we can, and shows up for each other’s hospital appointments. They’ve carried me through some of my darkest moments.

The most meaningful part of sharing my journey is helping others who are newly diagnosed and frightened, just like I once was. When doctors first said “Lupus,” I thought my life was over. I was wrong. My life didn’t end — it simply changed. And while it’s not the life I planned, it’s still mine, full of love, purpose, and resilience. And honestly — when does life ever go exactly as planned?