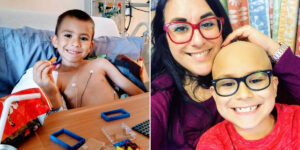
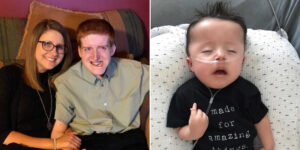
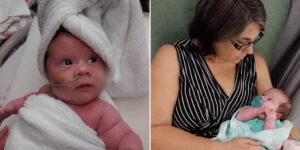
I’m a wife of 10 years to my very best friend, David, and we are blessed with three beautiful children here on earth, and two angel babies watching over us from heaven. In June 2017, we were surprised with the news that I was pregnant for the third time. It should have been joyful, but I was still on my Mirena IUD. The removal of the IUD triggered an early miscarriage at just four weeks, and we were left heartbroken, numb, and unsure how to process our grief. I slipped into deep depression, eventually returning to my previous antidepressants to cope, and decided to swear off IUDs entirely, starting the mini-pill instead.
A few months later, we went on a family vacation to Utah, hoping for a fresh start after months of heartache. We were laughing and enjoying ourselves, but I noticed unusual symptoms—emotional outbursts and sudden car sickness, something I had never experienced before. I initially blamed my antidepressants, but then realized, “When was my last period?” On our drive back to California, we stopped to buy a pregnancy test. It was positive.
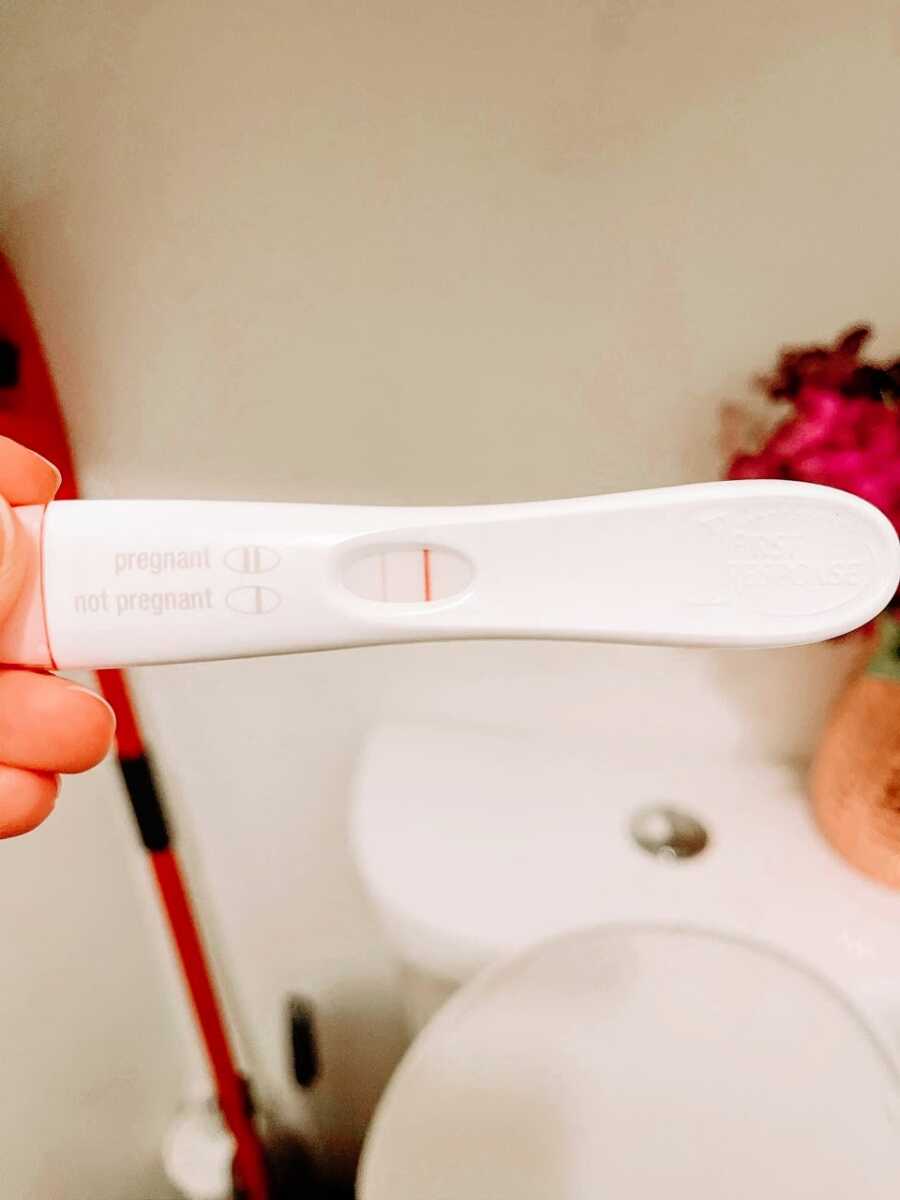
In September 2017, we discovered we were expecting our rainbow baby, a daughter, after two boys on earth and our angel baby in heaven. We named her Luna Aurora Panko—our moonlight in a dark time. But her arrival was far from easy. I battled Hyperemesis Gravidarum (HG), which left me in and out of hospitals with IV fluids and Zofran pumps.
By 16 weeks, my blood pressure had spiked dangerously. I was referred to a maternal-fetal medicine (MFM) specialist, where we learned I also had uterine notches in both the uterine and umbilical arteries—likely caused by my high blood pressure and severe obesity. At 24 weeks, I was diagnosed with preeclampsia, requiring weekly appointments. By 32 weeks, I was hospitalized until delivery, receiving constant magnesium sulfate drips, three IV blood pressure medications, and strict restrictions on food and water.

On March 11, 2018, the on-call MFM came to speak with David and me. She told us that if I became pregnant again, my weight, PCOS, and high blood pressure would put both me and the baby at severe risk, possibly fatal. She suggested a tubal ligation, warning that more than three Cesarean sections would be extremely dangerous, and left us with, “It’s your choice.” The pressure from doctors was overwhelming, and the lack of information about other options felt hurtful.

That night, exhausted, swollen, and doped up on magnesium, I was terrified. My thoughts raced: “I don’t want to die if I get pregnant again.” David worried he couldn’t raise three children alone. The next morning, just before my Cesarean Section, I signed the paperwork for a tubal ligation, a decision I would come to deeply regret.
Luna was born at 33 weeks on March 12, 2018, at 4:04 p.m., weighing 4lbs 4oz and measuring 17 inches long. She was perfect. Our family felt complete. She spent 32 days in the NICU, a familiar experience since our first son had been born at 32 weeks and spent 16 days there.
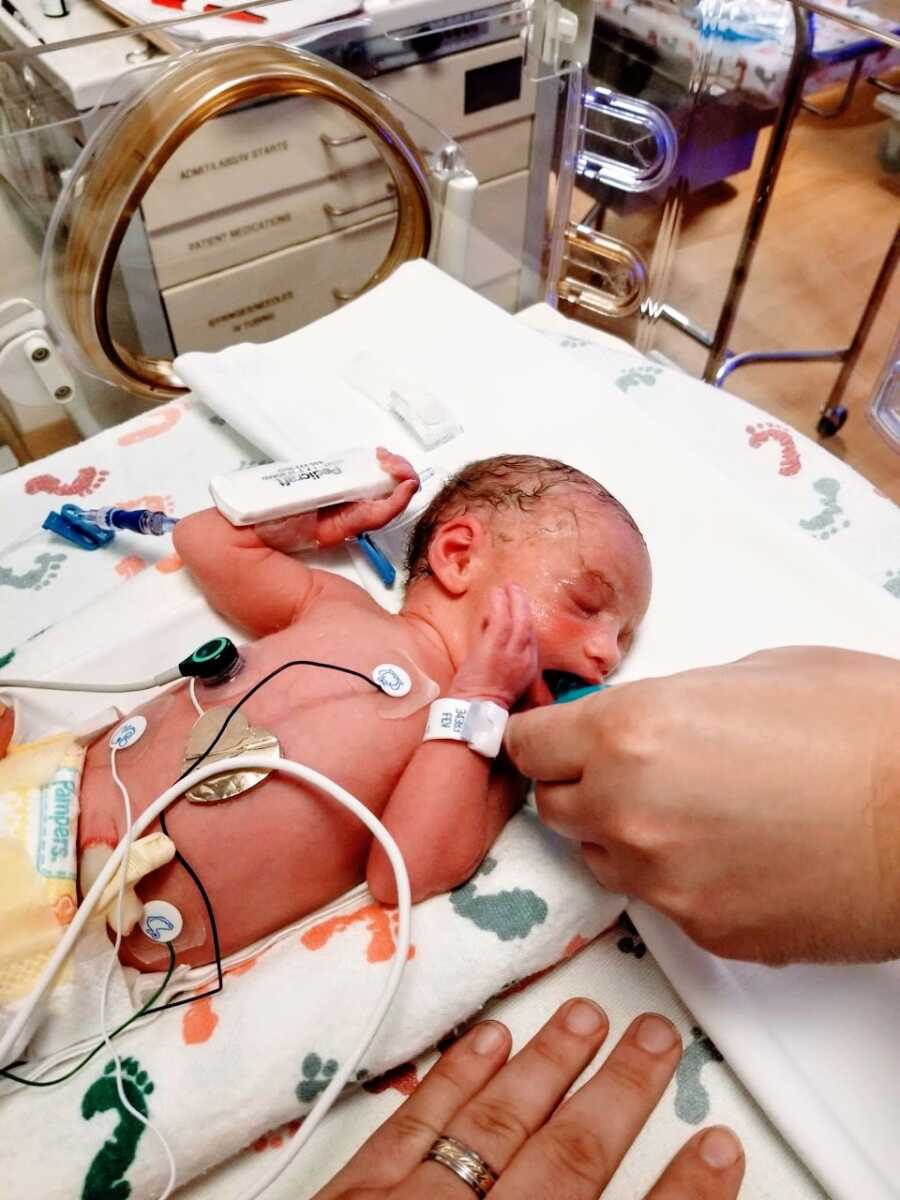
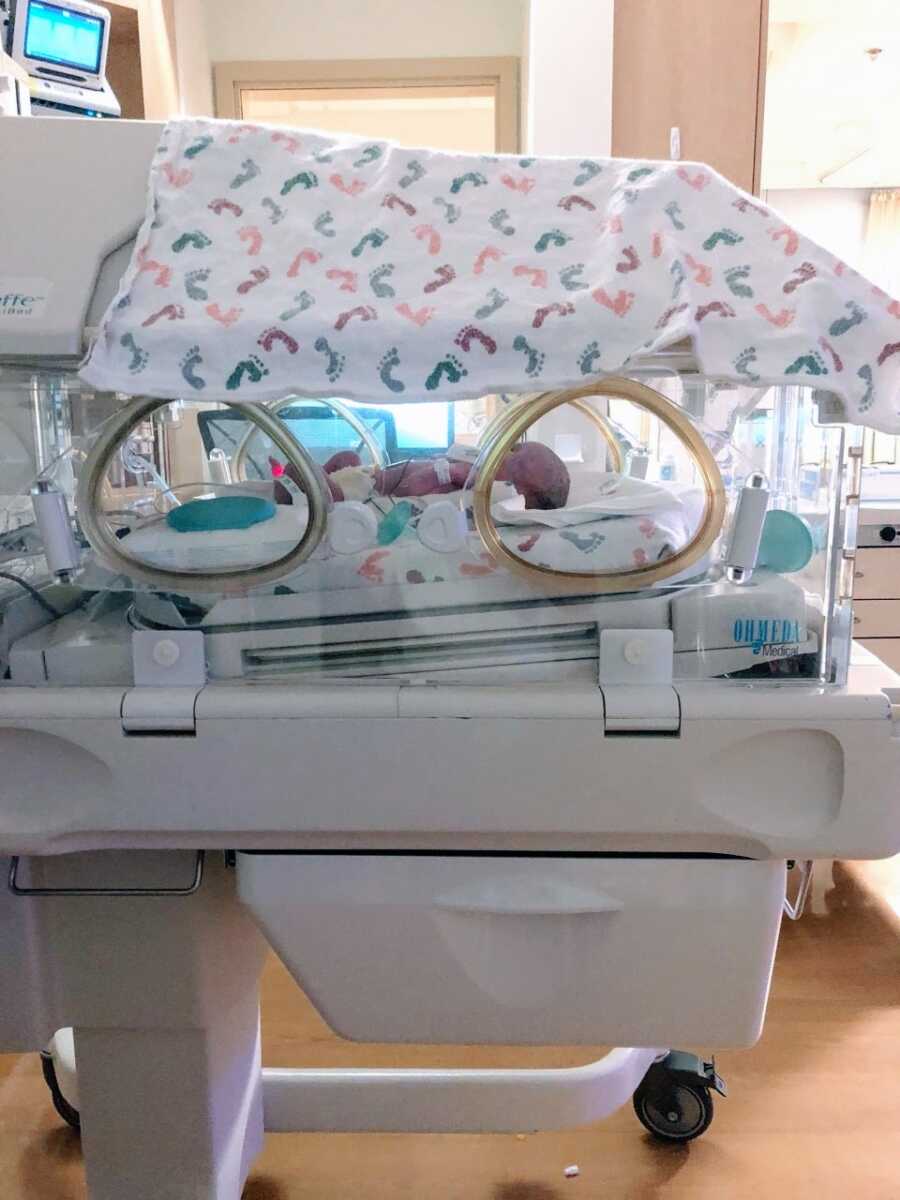
My recovery was grueling. I spent a week in the hospital, constantly walking back and forth to the NICU, unable to sleep next to my husband and newborn. After discharge, we moved to the Ronald McDonald House 15 minutes away from the NICU, while our older sons, just 2.5 and 5.5 years old, stayed with my parents. The separation, combined with my incision reopening, two hernias from surgery, and the emotional trauma of everything, plunged me into postpartum depression.
After Luna, a cascade of health issues began. My IIH flared up, migraines were constant, and I suffered severe night sweats, hot flashes, fatigue, anxiety, depression, PMDD, irregular periods with heavy bleeding and clotting, excruciating cramps, memory loss, pelvic pain, achy joints, and backaches—symptoms I had never experienced before. Even years later, I still live with many of these daily struggles, known as Post-Tubal Ligation Syndrome (PTLS), a reality doctors never warned us about. On top of that, my PCOS worsened, my ovaries and uterus slowly calcified, and I lived with two hernias from surgery.

My periods now last 8–16 days, leaving me weak, anemic, and bedridden much of the month. Nausea, stomach pain, and overall exhaustion have dominated my life. In the last year and a half, I’ve lost 100 pounds, which is a victory, but chronic illness makes daily life extremely challenging.

Despite all this, life threw us another curveball. On June 25, 2021—just two days before our son’s sixth birthday—I discovered I was pregnant. With my tied tubes and multiple health issues, the risks were immense: ectopic pregnancy, miscarriage, internal bleeding—risks no doctor had fully explained. Attempts to schedule appointments with OBs and MFMs were repeatedly denied. But after a week of hundreds of positive pregnancy tests, hope sparked. Could a miracle be possible?
Sadly, on July 4, at around 4.5 weeks, I began cramping and bleeding. I went to the ER, and our hopes were dashed—another miscarriage. Doctors were stunned at how this pregnancy had even occurred. The grief, confusion, and guilt were overwhelming. Questions haunted me: who would this baby have been? Another boy or girl? Would they have looked like their siblings or their daddy? The timing of loss doesn’t lessen its significance, and no one should grieve alone.
It’s been three months since that loss. Three months of missing a piece of our family puzzle. Three months of hoping for another miracle. We will get another chance. We will get our baby.
I deeply regret my decision to have my tubes tied, made in fear, pain, and under the influence of medication. There are options—IVF, Tubal Reversal—but costs are high, and access is limited. I share my story to help women understand all the possibilities before making such life-altering decisions. Your health, your choices, and your research matter. If you are suffering, your feelings are valid. You are not alone. My hope is that by speaking my truth, someone else may avoid the regret, guilt, and heartbreak I continue to navigate every day.