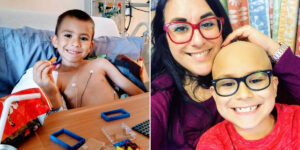
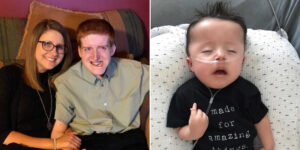
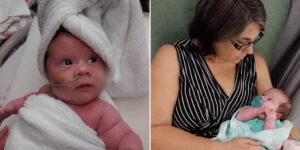
“‘Do you mind if I have someone else come take a listen?’ Little did I know how often I’d hear those words throughout my life.
From the time I was very young, I was always the patient who needed “extras.” Extra nurses, extra labs, extra tests. Each time a doctor would listen to my heart through a stethoscope, I’d watch their expressions shift. They’d listen carefully, frown, and then ask the same question: ‘Do you mind if I have someone else come listen to this?’ I always said, ‘Sure, I don’t mind.’ But I never understood why. Honestly, it was embarrassing.
I was born with a congenital heart disease (CHD) called Aortic Stenosis. For years, I didn’t even know it had a name. Until my teenage years, doctors just told me I had a murmur. When I was 14, I was referred to a cardiologist at Nationwide Children’s Hospital for an echocardiogram—or echo for short—which is an ultrasound of the heart. It allows doctors to examine the chambers, valves, arteries, and walls more closely. The average echo takes about an hour.
After the test, I met with my cardiologist and finally received a name for what had been affecting me all my life: I had Aortic Stenosis with a bicuspid aortic valve and significant regurgitation—blood flowing backward into the heart.
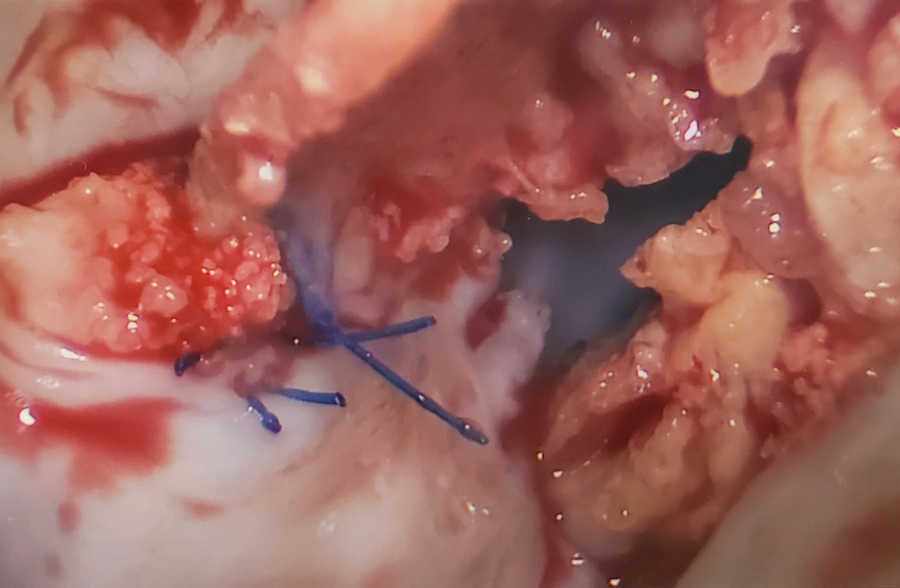
Aortic Stenosis is a condition where the aortic valve is narrowed. Normally, three flaps open and close to allow oxygen-rich blood to flow from the heart to the aorta and the rest of the body. In my case, two of my flaps had fused together during fetal development, leaving only one functioning flap. On top of that, calcification had built up, further limiting blood flow.
For years, I struggled with ordinary childhood activities. Running, sports, and even simple play felt impossible. I blamed it on asthma, though deep down I knew something more was wrong. By my teens, walking up a single flight of stairs could leave me winded. I was constantly tired and always cold. Despite these challenges, my teenage years were relatively normal: I had friends, I spent time riding and showing horses, graduated high school, and went to college.
In October 2011, at 18 years old, I returned to the hospital for my annual checkup. My results were similar to the previous year, showing no major changes, and I was told to return in two years instead of one. Everything felt fine, and I was optimistic.
But in December 2013, for my next checkup, things changed. I only had an echo that day and didn’t meet the cardiologist in person. A few days later, I was at a restaurant when my phone rang. It was him. The first word out of his mouth was, ‘Unfortunately…’ and in that instant, I felt as though I had been punched in the chest. At 20 years old, I learned I would need open-heart surgery to fix my diseased valve. I had so many questions, but shock left me speechless. I stepped outside, gave the news to my friend, then went home to my family, my head spinning with uncertainty and fear.
Within weeks, I returned for more testing: another echo, an EKG, and a stress test. I was used to the echo and EKG, but the stress test was new. I was hooked to monitors and asked to walk on a treadmill as the nurses gradually increased the speed and incline. Soon I was jogging. My chest tightened, my lungs burned, but I refused to stop. I was determined to prove to myself and the medical team that I could handle it. Eventually, they stopped the treadmill, and I stumbled off, winded, dizzy, and gasping for air.
Later, I met with my cardiologist. He explained the technical details of my valve, gradients, and blood flow. He told me I was walking the line between moderate and severe stenosis. Surgery wouldn’t happen until I hit the ‘severe’ stage, because insurance wouldn’t cover it otherwise.
I was livid. I had accepted that surgery was inevitable, and suddenly, I was told I wasn’t sick enough. I felt hurt, stressed, and angry—like a price tag had been placed on my life.
We discussed surgical options. I could attempt a valve repair using my own tissue—a newer procedure with uncertain longevity. I could receive a bioprosthetic valve from pig or cow tissue, which would last 5–7 years. There was the Ross Procedure, using my pulmonary valve to replace the aortic valve while implanting an artificial pulmonary valve. Or, a mechanical valve, which could last a lifetime but required lifelong blood thinners, complicating future pregnancies.
Over the following weeks, I weighed pros and cons with my family, doctors, and friends. I decided to try a repair first, keeping the mechanical valve as a backup.
When my valve finally reached the severe stage, my surgery was scheduled for December 4, 2014. I was a nervous wreck. Pre-op tasks done, my surgeon confirmed the plan: repair first, mechanical if necessary. My only question: ‘What’s the probability I’ll die?’ He reassured me with a calm smile: less than 3%.
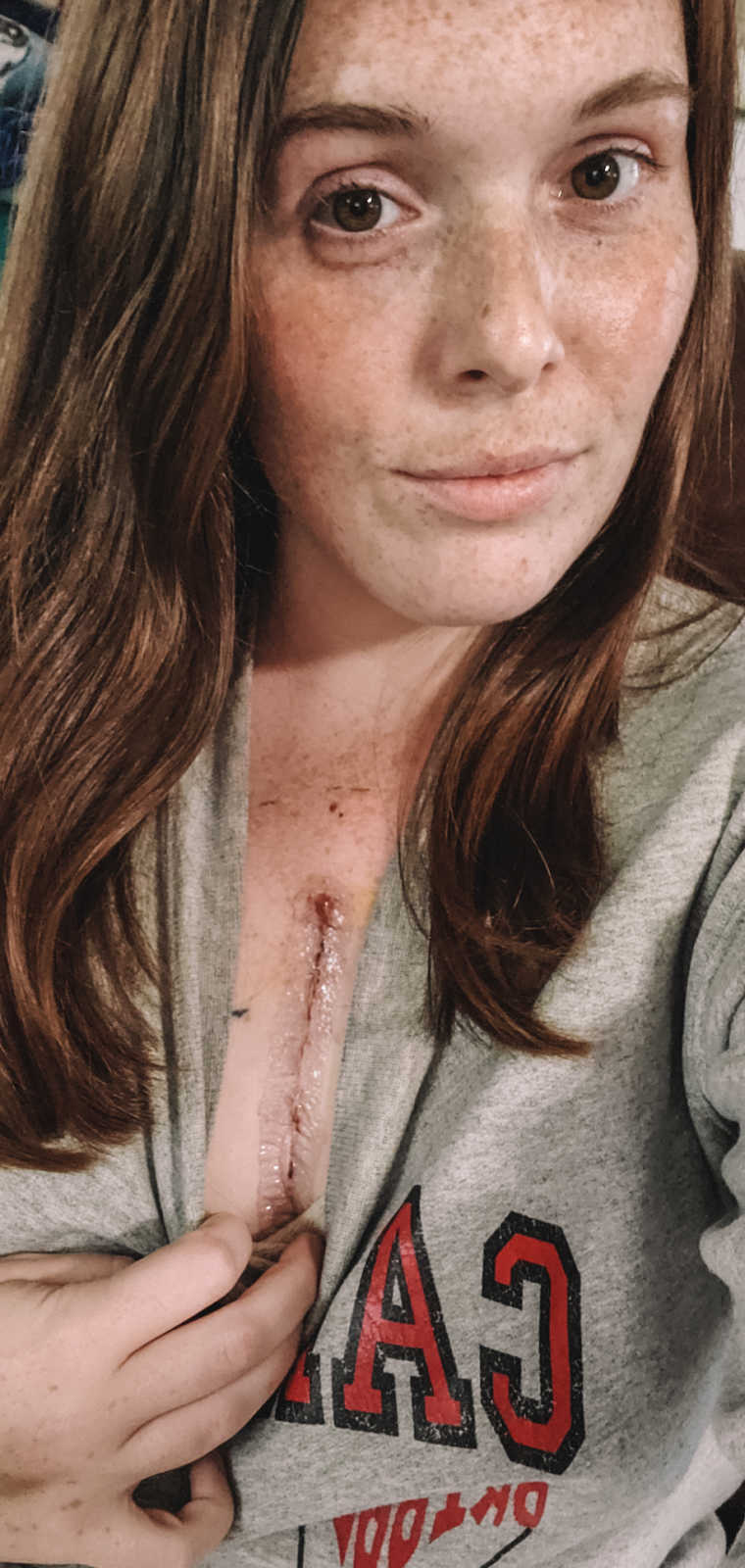
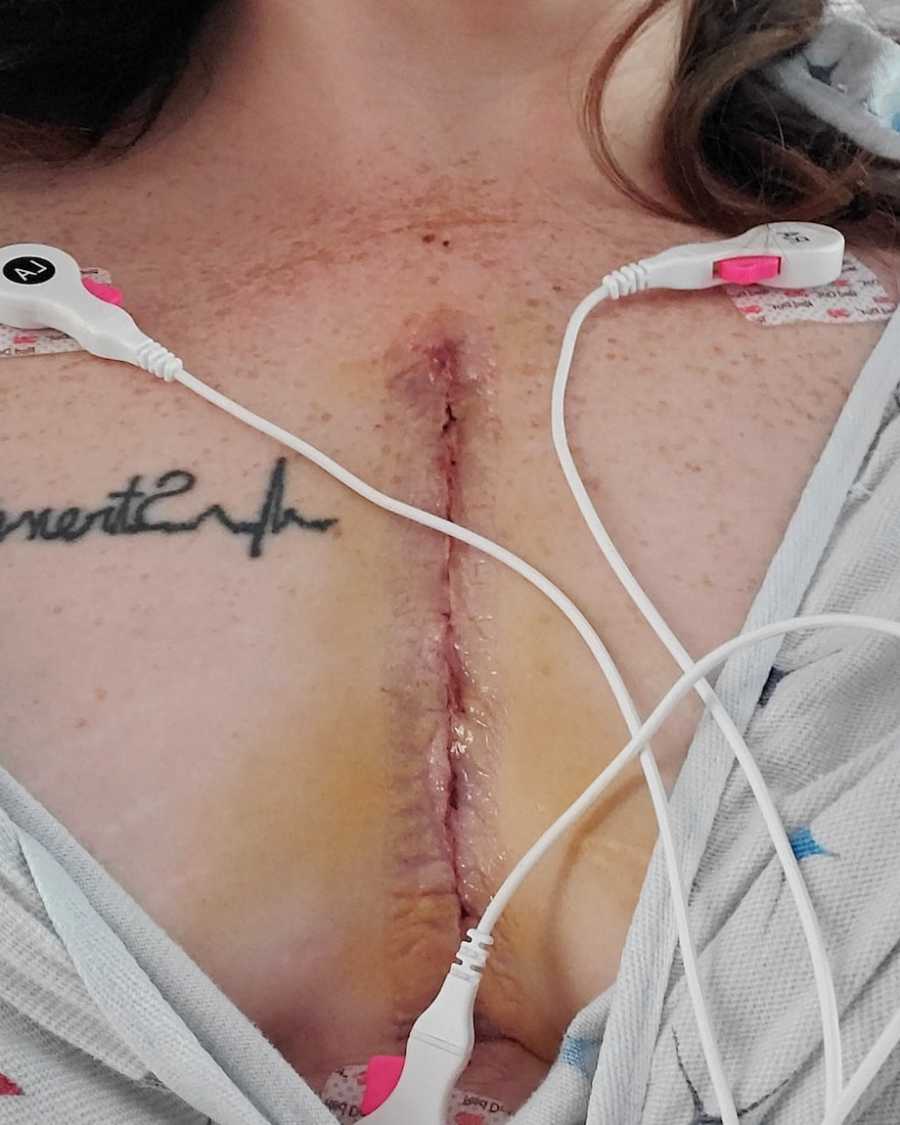
Nine hours later, I woke in the Cardiac ICU. Seeing my family and nurses, I thought, ‘I’m alive. I made it.’ Minor complications arose, but overall the surgery was a success. My repair included some cow tissue to replace damaged flaps.
Interestingly, the surgeon discovered I had a unicuspid valve, not bicuspid as previously thought. I spent four days post-op following every instruction—walking, showering, eating—and was finally discharged. Recovery went remarkably well, and I returned to work seven weeks later. For the first time, I had energy I’d never known. I could run, jump, and move freely. At every follow-up, my results amazed the doctors.
Two years later, I became pregnant with my first child. It was a high-risk pregnancy due to heart stress. At 35 weeks, I developed pre-eclampsia and was induced at 37 weeks. In August 2017, my husband and I welcomed our 5-pound, 13.5-ounce baby girl.
In May 2019, a routine checkup brought devastating news: my valve had calcified again. At 26, I faced my second open-heart surgery. Fear gripped me—this time, I had someone depending on me. Over a year, I underwent testing and monitoring, awaiting the right moment. Surgery options were limited this time, and I chose the mechanical valve to avoid a third operation.
On September 10, 2020, at 27, I had my second open-heart surgery. The day before, I recorded a video for my daughter, telling her she was my greatest joy, in case I didn’t make it home. The fear was suffocating.

Waking in the ICU, relief washed over me. I had made it. Though COVID-19 restrictions limited visitors, I video chatted with my daughter daily. Seeing her face when I returned home, I cried—overwhelmed with gratitude.

I completed 12 weeks of cardiac rehab and continue to exercise diligently. My outlook on life has transformed. Life is fragile, precious, and there is no time to waste being unhappy. Twice, my heart stopped and was restarted, and each time, I was reminded to cherish every heartbeat. I am on life #3, and every day I wake up grateful to celebrate it with the people I love most.”